Complete Guide to Progress Notes in Disability & Aged Care
Rob Scott

Progress notes are a vital part of a care delivery framework and a must-have for any care delivery team.
They reflect a client's movement towards their goals, as identified in their Individual Support Plans, and also represent a record of events on each shift or visit, thereby serving as a communication tool for staff.
By reading this guide, you can find out more about why progress notes are important, and what kind of information should be included in progress notes. You will also pick up valuable tips on how to write progress notes to a high professional standard.
What are Progress Notes in Disability Support?
Progress notes are documents created by support workers at the end of a shift and are an essential part of a Client's Personal File. In progress notes, staff succinctly record details that document a client’s status and achievements. Progress notes are a tool for reflecting on a client’s movement towards their goals, as identified in their Individual Support Plans. They also represent a record of events on each shift or visit, and act as a communication tool for staff and families.
As well as being used in disability support, progress notes may be used in aged care, community care, group programs, sheltered accommodation, and nursing homes.
Nursing Progress Notes
Nursing progress notes are vital for tracking patient care, communicating between healthcare professionals, and streamlining the process of writing these essential records. Here's how to approach them:
Timely Updates: They can be updated in real-time or at the end of a shift, helping to create a continuous and coherent picture of patient care.
Detail-Oriented: Include specifics about care, changes in condition, medication, and any incidents. The importance of accurate and detailed nursing notes cannot be overstated, as it ensures all team members are fully informed and can make sound clinical decisions.
Streamlining Process: With advances in technology and standardised methodologies, the process of writing nursing progress notes can be more efficient and consistent. By utilising appropriate tools and guidelines, nurses can focus more on patient care and less on administrative tasks. See 5 steps to streamline the process of writing nursing progress notes.
Legal Compliance: Understand that nursing progress notes function as legal and medical records and must be treated with accuracy and confidentiality. Precise and comprehensive documentation can also protect healthcare providers in legal matters.
Patient and Family Engagement: Share appropriate information with patients and their loved ones to foster trust and cooperation. Engaging with the patient and family helps in building rapport and facilitates more personalised care.
By focusing on these aspects, nursing professionals can enhance the quality of care, improve communication within the healthcare team, and ensure that the documentation process is both efficient and effective.
How are Nursing Progress Notes Used?
Just like in-home care, nursing progress notes are an essential record for improving the quality of care and support. They also function as legal and medical records and can be shared with both the patient or resident and their loved ones.
Nursing progress notes can be updated in real-time or completed at the end of the nurse’s shift. They should include details of a patient’s care, any changes in their condition or medication and any incidents.
Progress Notes in Aged Care: An Essential Tool
In aged care, progress notes help ensure older people receive consistent, high-quality care. They are a legal record that details the care the client receives, their health and any important changes. Day to day, they allow carers to communicate in-team about the client’s condition.
Progress notes are particularly helpful when clients have memory loss, as they serve as a tool for communication between the client, their loved ones and carers. Family and friends can receive regular updates about the client’s activities. Moreover, the contents of the progress notes can be used to navigate conversations without making the client feel uncomfortable about forgetting things.
Why Do We Write Progress Notes?
Progress notes are one of the most helpful tools in a carer’s or support worker’s arsenal. There are many reasons we write them, including:
1. Progress notes act as proof of service delivery
By recording progress notes, you can show clients, their loved ones and auditors that the promised services have been provided.
2. Progress notes are a legal record
Progress notes become part of a patient’s permanent legal record. They may be used in legal proceedings, audits and investigations. They also provide a paper trail in case of conflict or incidents, which brings us to our next point.
3. Progress notes can be used as evidence
Any incidents (whether proven or solely alleged) must be reported to the NDIS Commission, either directly or via a supervisor, manager, specified person, or member of the provider’s key personnel. You will probably also be asked to provide evidence of progress notes and/or a system for recording incidents during NDIS audits.
Reportable incidents and allegations include:
Injury
Alleged abuse and/or neglect by a worker, another participant, a family member, another service provider, visitors, members of the community, etc.
Unlawful sexual or physical contact or assault.
Sexual misconduct.
Unauthorised use of a restrictive practice.
Death
If you are unsure of whether to report an incident or allegation, report it! The relevant personnel will decide what (if any) action is needed.
4. Progress notes help you prepare the client’s plan review
Progress notes link the services provided and the client’s progress to their overall plan, client goals and strategies.
Information from progress notes can be used to write client NDIS progress reports, which usually need to be submitted every 12 months. These reports help the NDIS (or aged care decision-makers) with progress and care plan reviews. In turn, these then help guide the carers whose work it is to implement participant goals.
Discover how to measure the outcomes on the NDIS website.
5. Progress notes are a tool for sharing information
Progress notes can be used to share information between carers, families and coordinators (including team leaders and managers). This allows all interested parties to stay abreast of changes in patient status, routines and needs.
Progress notes can also act as handover notes for next shift staff. For in-home services, they play a vital role in ensuring transparency of care between care teams, as well as for primary carers.
Here are some simple examples that demonstrate how sharing information recorded during care visits can be helpful:
Sharing information between different carers
A carer working with a patient in the morning records in a progress note that the patient has not eaten their breakfast. The carer coming on shift with the same patient in the afternoon has access to that information and can make sure that the patient eats lunch.
Sharing information between care workers and families
A care worker goes out shopping with a patient with dementia and records the experience, including what was purchased. Having read the notes, the patient’s family can use the information as a point of conversation.
Without context, it may be hard for a dementia patient to remember the morning visit to the shop, and it could frustrate them when the topic is raised. Reading the progress note, however, will enable a family member to ask detailed questions, such as: “How was shopping? I understand you bought new cushions, what colour are they?” This creates a more rewarding experience for both the patient and their family.
How to Write Progress Notes
A progress note is by no means the entire record of the visit. It is simply a snapshot of what transpired, including the most significant factual information. If the carer is already familiar with the client’s routines and behaviour, the main point is to note any deviation from the client’s normal routines and patterns.
Progress notes are partly generic in nature; for example, comments on a patient’s physical state and emotional well-being are likely to be appropriate whether the setting is mental health care, disability care, dementia care, or any kind of nursing context. Beyond this, progress notes should also relate to a client’s individual plan; to their individual goals and strategies.
All progress notes must include:
Your name.
The date and time.
Details of any reportable incidents or alleged incidents, including those involving peers or others, and details of witnesses if there are any.
Other types of information that it may be appropriate to record in progress notes, depending on the specific home care situation, include:
Visits from health professionals.
Changes emotional wellbeings.
Carer interventions and assistance given.
Changes in behaviour.
Degree of participation in activities.
Behaviour of concern (what happened before, during and after).
Reactions to medications.
Concerning changes in physical appearance.
Dietary notes.
Here are some important guidelines to consider when making progress notes:
Progress notes should be recorded at the end of every shift.
Progress notes can be written by hand or typed.
Write down events in the order in which they happened.
Include both positive and negative occurrences and anything out of the ordinary.
Record errors made by caregivers - even your own errors!.
Keep in mind the goals in the client’s plan. You may wish to work from different progress note templates for different patients.
Write concisely, so that others can easily scan the information. At the same time;
Notes need to include enough information so that others can understand what happened.
Where significant, state what occurred before, during and after an incident.
Use plain language that any adult would be able to understand (even if they have no specialist knowledge, speak English as a second language, or have a learning disability).
Consider using the STAR model to record information: Setting, Trigger, Action, Result.
Be specific. For example: “At 3:45 pm Jane’s temperature was 39 degrees”, not just, “Jane had a fever this afternoon”.
Accurately describe the types of assistance given during each activity. Eg. Verbal cues, or hand-over-hand assistance.
Write using the ‘active voice’ rather than ‘passive voice’. The active voice places the focus on the doer of the action.
Information should be objective, not subjective. What did you see/hear/say/do? Record concrete, factual information. Do not include your opinions about the facts. (For more help with how to write progress notes objectively, see this NDS workbook
Here are examples of objective and subjective writing, taken from the same workbook:
Example of objective writing:
“At 3.30 pm Marcella returned from a walk to Albert Street Park and she was holding her right arm against her body. She had a graze and bruise on her right arm. Marcella said a dog had jumped on her when she was sitting on the grass at the park. She said she had been frightened and that her arm was sore.”
Example of subjective writing:
“Marcella must have bumped into something when she went on a walk to Albert Street Park, as she has grazed skin and a bruise on her arm. She was holding her arm and looked unhappy.”
Different Model Approaches to Writing Progress Notes
SOAP Method
SOAP notes are a commonly used method for recording progress, particularly in medical and healthcare settings. SOAP stands for Subjective, Objective, Assessment, and Plan:
Subjective: This includes the patient's expression of how they feel, including symptoms and concerns.
Objective: Record observable and measurable data, such as vital signs, test results, and physical examination findings.
Assessment: This is the professional's interpretation of subjective and objective information, leading to a diagnosis or identification of the problem.
Plan: Detail the planned treatment, interventions, or actions to address the issue.
SOAP notes promote consistency and clarity, ensuring that critical information is not overlooked. For a more detailed explanation, view the complete guide to SOAP notes.
STAR Method
The STAR method is a structured approach to documenting or describing situations, often used in interviews, performance management, or clinical settings. STAR stands for Situation, Task, Action, and Result:
Situation: Begin by describing the context or setting in which a specific event took place. This should provide enough detail for the reader to understand the background.
Task: Explain the task or challenge that was at hand. This could be a problem that needed solving, a goal that needed achieving, or a responsibility assigned to an individual or team.
Action: Outline the actions that were taken to address the task or challenge. This should include specific steps, decisions, or behaviours, not general statements.
Result: Conclude with the result of the actions. This could include outcomes, what was achieved, what was learned, or any impacts on broader goals or objectives.
The STAR method helps to create clear and concise narratives, whether in clinical progress notes, performance reviews, or when describing experiences. By focusing on these four elements, professionals can ensure that their descriptions are both comprehensive and focused on essential details.
In a clinical setting, STAR can be used to detail interventions, patient interactions, or responses to particular treatments or behaviours. It helps in creating a clear and objective picture of events, decisions, actions, and outcomes, promoting effective communication and documentation.
Other Progress Note Methodologies
When it comes to methods used to write progress notes, SOAP and STAR are the more popular models used by NDIS and aged care providers. However, there are other methodologies and frameworks worth mentioning that may vary depending on the healthcare setting, patient population, or specific clinical needs:
DAR (Data, Action, Response): This is a streamlined and focused method of documentation, focusing on the data (observation), action (intervention), and response (outcome).
SBAR (Situation, Background, Assessment, Recommendation): Often used in nursing handoffs, this method helps ensure that all necessary information is conveyed in a clear, concise manner.
APIE (Assessment, Plan, Implementation, Evaluation): This method represents a care planning cycle and is used to ensure a systematic approach to patient care.
CBE (Charting by Exception): Rather than documenting everything, CBE focuses on documenting deviations from established norms or expected findings, making the documentation process more efficient.
FOCUS Charting (F-DAR: Focus, Data, Action, Response): A patient-centered approach where the focus might be a patient strength or a problem/need. It integrates assessments and interventions.
POMR (Problem-Oriented Medical Record): This method organizes information around a patient's specific problems, making it easier to track the progress and outcomes related to individual issues.
Narrative Charting: This is a more traditional and chronological way of documenting, telling a story in a logical sequence. It's less structured than other methods but can provide a more detailed picture of a patient's experience.
Critical Pathway Method: Often used in managing specific clinical scenarios, this method integrates an evidence-based care pathway to guide the care process.
GIRP (Goal, Intervention, Response, Plan): Similar to the DAR method, but with an added emphasis on the goal that guides interventions and evaluations.
e-Health Tools: Many healthcare settings are using integrated electronic health records (EHRs) and other e-health tools that often have built-in templates and guidance based on best practices.
Ultimately, different methods may be more appropriate depending on the particular context, whether it's a specific healthcare setting like mental health, emergency care, or chronic disease management. The choice of method could also be influenced by regulatory requirements, the need for interdisciplinary communication, or specific goals like improving efficiency or patient engagement. An understanding of these different methodologies allows healthcare professionals to select the most appropriate tool for their specific situation.
Writing Helpful NDIS Progress Notes
The National Disability Insurance Scheme (NDIS) demands reporting to ensure the quality of care. Writing helpful NDIS progress notes is crucial for reflecting a client's movement towards their goals and in accordance with their individual plans.
Understand the Goals: Align the progress notes with the client's specific NDIS goals.
Be Detailed: Include any changes in condition, behaviour, or medication, as well as incidents.
Compliance with Standards: Ensure that your notes comply with NDIS standards for reporting and accountability.
Client-Centred Approach: Focus on the client’s needs, preferences, and individuality.
Importance of Client and Family Involvement:
In the realm of the NDIS and disability support, involving clients and their families in the process of care is paramount. This collaboration extends to the creation and review of progress notes, which can greatly enhance the care provided. Here's why client and family involvement should be considered:
Building Trust: When clients and their families are involved in the development of progress notes, it fosters a sense of trust and partnership. They become active participants in care, rather than passive recipients.
Enhancing Communication: Collaborative efforts ensure that communication lines are open and transparent. Families can offer unique insights into a patient's condition, preferences, and needs, which can be critical in tailoring care.
Ensuring Accuracy: Including clients and families in the review of progress notes can ensure that the information documented is accurate and reflects the patient's true condition and experience. It also helps in identifying any misunderstandings or gaps in information.
Improving Outcomes: Family engagement leads to a more holistic view of the patient's needs. By including their perspectives, care plans can be designed more effectively, leading to better patient outcomes.
Empowering Clients: Involvement in the progress note process empowers clients to take an active role in their care. It promotes self-management, responsibility, and aligns the care with their values and preferences.
Compliance with Standards: Many healthcare frameworks and regulations emphasize the importance of patient-centered care. Involving clients and families in progress notes aligns with these standards, promoting quality care.
Supporting Emotional Well-being: The sense of inclusion and partnership can ease anxiety and enhance the emotional well-being of both clients and their families. Knowing that their voices are heard and respected can make a significant difference in their experience.
Resolving Conflicts: In cases where there are disagreements or concerns, involving clients and families in the discussion around progress notes can lead to resolution and understanding, mitigating potential conflicts.
Cultural Sensitivity: Every family has its unique cultural norms and values. Incorporating these into care planning and documentation helps in delivering culturally sensitive and appropriate care.
Legal and Ethical Alignment: In some jurisdictions, client and family involvement might not just be good practice but also a legal requirement, ensuring that the care provided aligns with legal and ethical standards.
Good vs Bad Progress Notes
Understanding the difference between good and bad progress notes is essential for maintaining high standards of care:
Good Progress Notes:
Objective and factual.
Clearly tied to the client's individual goals and care plan.
Comprehensive but concise.
Follow accepted formats like SOAP.
Regularly updated, with accurate timestamps.
Bad Progress Notes:
Vague, ambiguous, or incomplete.
Lacking in specific details or connection to the client's goals.
Subjective or opinionated.
Irregularly updated or lacking in timeliness.
Non-compliant with legal and professional standards.
Using Software To Simplify Progress Notes
Modern healthcare and caregiving can benefit from using specialised software to handle progress notes:
Real-time Updates: Allows caregivers to record and access notes instantaneously.
Secure Storage: Ensures that all records are kept safely and in compliance with legal requirements.
Ease of Use: Features like speech-to-text can make the process of writing notes quicker and more accurate.
Inter-Team Communication: Facilitates seamless sharing of information between care teams, supervisors, and family members.
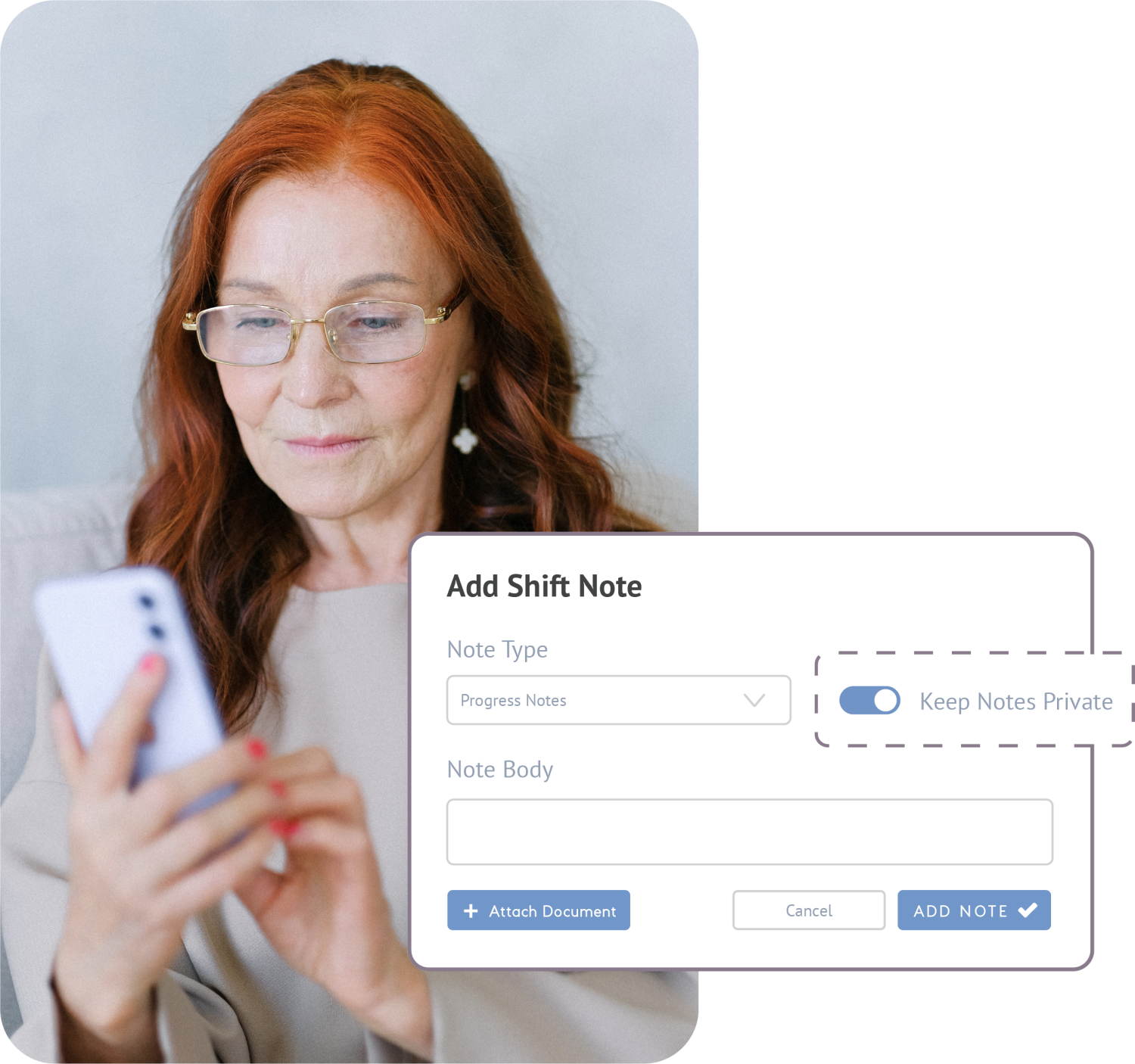
How is ShiftCare Revolutionising Progress Notes?
Recording and sharing ongoing progress:
ShiftCare’s Progress Notes provide a daily account of each client, their health and welfare and any developments in their care. This information can then be accessed by all carers and support providers, and in turn, enable them to better meet the client’s needs.
What’s more, it’s easy for carers to record and share progress via the ShiftCare app. Speech-to-text technology allows carers to quickly record progress notes. The voice notes are automatically transformed into text ready to be submitted.
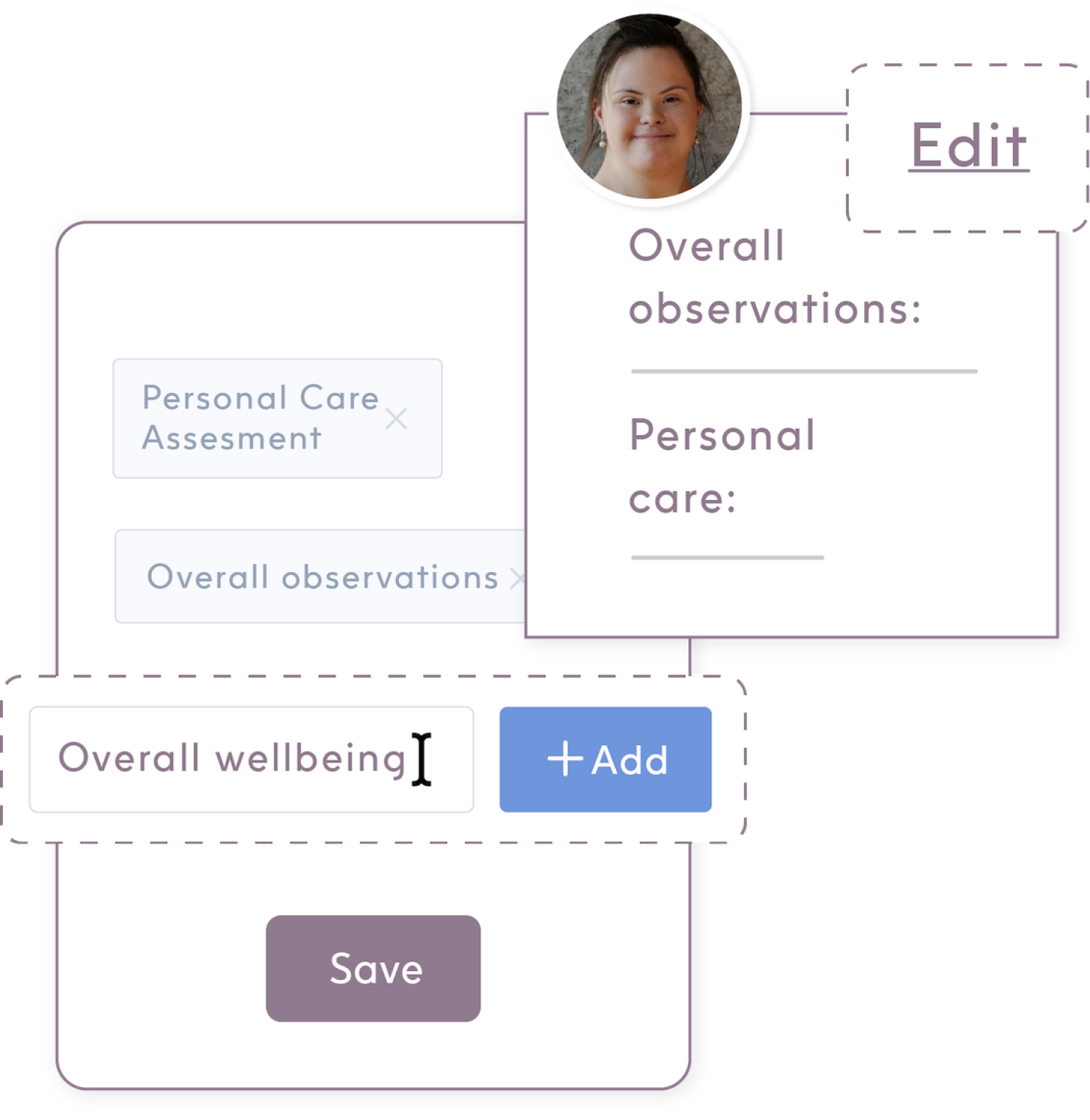
Customisable notes templates
Every team may have varying priorities, and each participant presents unique needs. By providing the ability to create and customise templates, we facilitate a streamlined process for teams to capture and disseminate the crucial information they require.
This tailored approach ensures that all members can function at their optimal level, focusing on individualised care and fostering effective communication within the team.
Smooth & immediate transfer of handover notes:
Carers and support providers can access progress notes on their phones as soon as they’ve been submitted. This gives them an instant update on a client’s condition and any ongoing issues. Since it’s all digital, there’s no need to coordinate a handover of physical documents. Instead, sharing these notes between teams in real-time means no problem will be overlooked.
Private notes
Manage the accessibility of notes by controlling who can view them. This process ensures that privacy is maintained while simultaneously allowing for the sharing of notes with specific individuals as needed.
Such careful regulation not only adheres to confidentiality requirements but also facilitates precise communication between designated healthcare professionals, enhancing the overall care process.
ShiftCare keeps records of progress notes for audit purposes:
Auditors will inspect progress notes to check that carers have visited clients at the correct times and all concerns and incidents have been appropriately reported and handled.
With the ShiftCare app, you’ll be well-prepared for an audit. All your progress notes and other important documentation will be available in one place. Records are stored securely on our server, and there is no risk of information loss, theft or damage.
Progress notes in disability, aged care and nursing aren’t just a legal requirement. They’re also a tool that will help your business run smoother by ensuring good communication between team members. Most importantly, progress notes enable you to provide high standards of care and monitor clients’ needs.
FAQ's
What is the difference between SOAP and STAR notes?
SOAP notes focus on Subjective, Objective, Assessment, and Plan, making it suitable for healthcare progress tracking. STAR notes, on the other hand, deal with Situation, Task, Action, and Result, often used for reflective practice or performance evaluation.
How can software tools help in writing progress notes?
Software tools can streamline the process of writing notes by providing templates, automating repetitive tasks, ensuring legal compliance, and enhancing collaboration between healthcare professionals. They can also enhance the privacy and security of the notes.
What are nursing progress notes, and why are they important?
Nursing progress notes are detailed records of a patient's care, changes in condition, medication, and incidents. They are crucial for real-time communication between healthcare professionals and provide legal documentation of care. Accurate and detailed nursing notes are essential for patient safety and continuity of care.
Why is client and family involvement important in healthcare?
Involving clients and family in healthcare decisions fosters trust, cooperation, and partnership. It allows for personalised care, respecting the patient's values and preferences, and often leads to better outcomes and patient satisfaction.
Are there specific legal considerations for writing progress notes?
Yes, progress notes must comply with legal requirements related to patient confidentiality, consent, and professional standards. Errors or omissions can have legal ramifications, emphasising the need for accuracy and thoroughness in documentation.
How can I choose the best method for writing progress notes for my setting?
Choosing the best method depends on the context, patient population, clinical needs, regulatory requirements, and personal preferences. Understanding different methodologies like SOAP, STAR, DAR, SBAR, etc., allows healthcare professionals to select the most suitable method for their specific situation.
Can patients access their own progress notes?
Patients have the right to access their medical records, including progress notes. This access encourages transparency and partnership in care, although some limitations and processes may apply depending on local laws and policies.
How do you write progress notes for NDIS?
Writing progress notes for NDIS requires a clear understanding of the individual's goals, the services provided, and the outcomes achieved. It should include specific details, be written in a professional tone, and follow the guidelines set by the NDIS.
Do support workers need to write progress notes?
Yes, support workers often need to write progress notes to document the care and services provided to individuals. These notes are essential for communication within the healthcare team and for maintaining continuity of care.
What is a progress note template?
A progress note template is a pre-formatted document used by healthcare professionals to ensure consistency and completeness in recording patient care. It may include specific fields for various aspects of care, such as symptoms, interventions, and outcomes, and can streamline the documentation process.
To discover how ShiftCare’s progress notes feature can revolutionise your business, sign up for a free trial.
 au
au